|
The study examined demographic and socio-economic factors that may influence pharmaceutical services (PS) in underserviced communities of the West Rand District, Gauteng Province, South Africa. A quantitative survey was conducted using structured questionnaires administered to the general public (n = 2014) in Bekkersdal, Kagiso, Mohlakeng, Munsville and Diepsloot townships. The questionnaire explored demographic details, employment and education status, income levels, payment methods and convenience of services. Of the respondents, 54.0% were women, 52.0% were unemployed; 65.0% had secondary education or higher and > 70.0% had no income or earned < R1000 p.m. Unemployment was higher amongst women. Only 13.9% of respondents had medical aid membership, which influenced their choice of health provider, with the exception of pharmacy services which are not affected by medical aid membership. Medical aid members were, however,
more able to pay. Employment status and education also influenced the choice of provider, with most of the employed (66.0%) and educated (64.4%) preferring a pharmacy or GP. On pharmacist gender, 47.5% of respondents had no preference, 27.6% preferred male pharmacists, whilst 24.9% preferred female pharmacists. Men with preferences preferred male providers (77.0%), whilst female respondents preferred female providers (69.3%). Respondents with no formal education and those with low or no income expressed higher gender preferences rates than those with formal education or higher income, respectively. Thus, access to PS was influenced by gender, age, family income and education level. Whilst medical aid membership had no influence on access to PS, it influenced ability to pay. These factors should be considered by those wishing to offer PS in such areas.
Toegang tot farmaseutiesedienste (FD) bly ‘n uitdaging in minderbevoorregte gebiede. Die huidige studie het demografiese- en sosio-ekonomiese faktore ondersoek, wat FD kan beϊnvloed in onder-bediende gemeenskappe van die Wes-Rand Distrik, Gauteng Provinsie, Suid-Afrika. Om te bepaal watter faktore toegang tot FD in vyf dorpsgebiede aan die Wes-Rand beïnvloed. Kwantitatiewe opnames met behulp van gestruktureerde vraelyste wat aan die algemene publiek (n = 2014) in Bekkersdal, Kagiso, Mohlakeng, Munsville, en Diepsloot dorpsgebiede uitgedeel is. Die vraelys het areas insluitende demografiese besonderhede, indiensneming- en opvoedingstatus, inkomstevlakke, metodes van betaling, en die gerief van die apteekdienste ondersoek. Daar was 2014 respondente (54.0% vroulik); 52.0% was werkloos; 65.0% het sekondêre of hoër onderwysopleiding; en > 70.0% het geen inkomste of verdien < R1000 p.m.
Werkloosheid was hoër onder vroue, ongeag van vlak van opvoeding. Slegs 13.9% van die respondente het mediese fonds-lidmaatskap. Mediese fonds-lidmaatskap beïnvloed die keuse van gesondheidsverskaffer, maar toegang tot die apteekdienste is nie geraak deur mediese fonds-lidmaatskap nie. Mediese fondslede was egter meer in staat om te betaal. Die keuse van ‘n verskaffer is deur indiensneming- en opvoedingstaus beïnvloed, met die meeste van die respondente wat werksaam was (66.0%) en die meer opgevoedes (64.4%), wat ‘n apteker of ‘n algemene praktisyn verkies het. Ten opsigte van die apteker se geslag het 47.5% van die respondente geen voorkeur gehad nie, 27.6% het manlike aptekers verkies, terwyl 24.9% vroulike aptekers verkies het. Mans met voorkeure het manlike verskaffers verkies (77.0%), en vroulike respondente het vroulike verskaffers verkies (69.3%). Respondente met geen formele opleiding, en diegene met ‘n lae of geen inkomste het hoër geslagsvoorkeur resultate getoon. Toegang tot FD is beïnvloed deur geslag, ouderdom, gesinsinkomste en vlak van opvoeding. Mediese fonds-lidmaatskap daarenteen het geen beduidende invloed op die toegang tot FD gehad nie, maar wel op die vermoë om te betaal. Hierdie faktore moet in ag geneem word deur diegene wat belangstel om FD in soortgelyke gebiede te verskaf.
Problem statement
Whilst the South African health system has undergone a lot of changes since the first democratic elections in 1994, there remain areas that are poorly serviced by all health providers. Pharmaceutical services remain unevenly distributed between urban, wealthy areas and poverty-stricken rural and township areas. The factors that influence access to pharmaceutical services in such underserviced areas in South Africa
apparently have not been studied, which may limit expansion of services in those areas.
Aims of the study
The aim of the present study was to determine the factors that influence access to pharmaceutical services and care in underserviced
areas of the West Rand District, in the Gauteng Province of South Africa.
Research objectives
The research objectives of the present study were as follows:• To establish the influence of demographic factors such as sex, language, education level and employment status on access and utilisation of pharmaceutical services in the underserviced areas of the West Rand. • To determine the influence of income and different methods of payment (for service) on access and utilisation of pharmaceutical services in the underserviced areas of the West Rand. • To assess the views of community members on access and utilisation of pharmaceutical services compared to other health care services such as primary health care clinics and general practitioners in the West Rand. South Africa is a diversified country with eleven official languages and many ethnic groups. During apartheid (generally, the period from 1948 to 1994), the Group Areas Act [Act No. 41 of 1950) (Parliament of South Africa 1950)] ensured, on the basis of race, ethnic groups, language and colour, that certain populations did not receive quality health care, including pharmaceutical services. Those inequities remain largely in place despite the fact that it has been more than 17 years since the country’s first democratic elections in 1994. Access to services may also be affected by factors such as socio-economic status, language, religion and cultural belief systems (Harrison, Bhana & Ntuli 2007), all of which are relevant to the diverse South African population mix. Health care in South Africa comprises two sectors: the public sector, which serves 80% population of the country and consumes 20% of the country’s health expenditure, and the private sector, which serves approximately 20% of the population at 80% health expenditure (Dambisya 2005; Tshabalala-Msimang 2001). The distribution of all resources – financial and human – follows the same pattern (Blecher & Harrison 2006) and evidence suggests that pharmaceutical services are in short supply in poor rural areas, whereas urban, wealthy areas are overserviced by pharmaceutical service providers (Barron 1998; Van Rensburg & Pelser 2004). The World Health Organization (WHO) consultative group of 1988 stated that effective medical and primary health care can be practiced only where there is effective medicine management (WHO 1988). The pharmacist is therefore a vital member of the health care team and the nature and access to pharmaceutical services may be a proxy for the quality of health services in a particular area. The role of a pharmacist, as defined in the National drug policy of South Africa (Department of Health 1996), includes aspects such as quality assurance and safety. And yet, as noted above, many rural, poor areas do not have access to pharmacists or pharmaceutical services (Van Rensburg & Pelser 2004). The present study was intended to contribute to the discourse on the need to increase pharmaceutical services in such underserviced areas.
Significance of the study
There remains a significant maldistribution of pharmaceutical services between urban and rural or township areas and little is known about the factors that influence access and utilisation of such services in those underserviced areas. The present study contributes to bridging the knowledge gap on the factors influencing access and utilisation of pharmaceutical services in underserviced areas and may
therefore contribute to the expansion of those services to disadvantaged areas.
|
Research method and design
|
|
Design
This was a prospective, cross-sectional study using a structured questionnaire targeted at members of the public in underserviced areas of the West Rand District.
Materials
The five townships selected for this study comprised a combined population of 275 786 people. From this, it was calculated that the minimum sample
size of 2000 was required, which led to a total of 2014 participants completing the questionnaire.
Data collection methods
Structured questionnaires were completed by 10 field workers during personal interviews with participants. The field workers were trained in techniques for administration of the questionnaire and equipped to address queries from the respondents. Prospective respondents were approached using an opportunistic strategy, based on convenience, at popular meeting areas such as taxi ranks, churches, outside school grounds and outside shopping areas. Deliberate effort was made to exclude the respondents at or near a pharmacy or any other health facility because it was felt that this may bias the sampling. The questionnaire covered a number of factors that may influence access to the pharmaceutical services, such as age, gender, home language, nationality, level of education, medical aid membership, employment status, means of transport, family income, expenditure on health care, gender of the service provider, language of service, patient privacy and the choice of provider. The questionnaire was translated into eight languages, namely, isiXhosa, isiZulu, Sepedi, Southern Sotho, Venda, Tsonga, Tswana and Ndebele to ensure that each respondent was engaged using his or her preferred language. Completion of the questionnaire took on average 30 min.
Data analysis
Data were analysed using SAS® 9.1 software (SAS 2008). Summary statistics were generated for the responses to the major questions and independent variables, such as gender, age, home language, education levels and nationality, were tested for association with the responses on choices such as preferred language of interaction with pharmacist and preferred pharmacy opening hours. The significance of the cross-tabulations of the various responses was tested
using the Chi-square test, with p < 0.05 as the limit of significance.
Context of the study
The West Rand District of the Gauteng Province was the site for the study. This is predominantly a mining community, with a diversified population speaking many languages. Five townships were used within the broad study site: Bekkersdal in Westonaria,
Mohlakeng in Randfontein, Kagiso and Munsieville in Krugersdorp and Diepsloot in Fourways.
There were 2014 respondents from the five study sites. There were more female respondents (n = 1088, 54.0%) than male (n = 926, 46.0%). The age distribution of the respondents was as follows: 44.1% (n = 887) were 15–30 years of age, 35.6%
(n = 697) were 31–45 years of age, 13.5% (n = 271) were 46–60 years of age, 5.7% (n = 114) were 61–80 years of age and 2.1% (n = 43) were older than 80 years. Most of the respondents were South African nationals and the majority (n = 1038, 52.5%) indicated that isiXhosa was their home language, whereas 32.5% (n = 643) indicated that it was South Sotho and 10.0% (n = 198) stated that it was isiZulu. The other languages indicated by 5.5% (n = 111) of the respondents included Sepedi, Setswana and Ndebele. More than a third of respondents had no or little (primary) education, whereas more than half the respondents (n = 1041, 52.0%) reportedly had a secondary school education and only 13.0% had tertiary education or postgraduate training (Figure 1). A negligible number (n = 13; 0.6%) of respondents did not indicate their highest level of education. There were no gender differences in education status of respondents. A minority of respondents (39.8%) were employed full-time, self-employed or were engaged in part-time work. Employment status was associated with gender: 40.7% of male respondents were unemployed compared to 64.3% of female respondents, 32.0% of male respondents and 13.6% of female respondents were in full employment, whilst 12.6% of male respondents and 10.0% female respondents were self-employed. The respective figures for part-time employment were 7.7% and 6.5%. Overall, female respondents were more likely to be unemployed (p < 0.001), regardless of
education level.
Language preferences
On the preferred language for consultation, two major options emerged (Table 1): 938 (46.7%) respondents indicated that they preferred to communicate with their pharmacy service providers in isiZulu, whereas 664 (33.1%) preferred Sotho; the remaining 405 (20.2%) indicated other options including English (n = 132, 6.6%), Tsonga (n = 87, 4.3%), isiXhosa (n = 105, 5.2%), and Tswana (n = 92, 4.6%). For 127 (6.3%) respondents, the language did not matter. There were significant differences between home language and preferred language for consultation (p < 0.001) (Table 1). Most of those who indicated isiZulu as their home language preferred to consult in isiZulu, whilst those for whom isiXhosa was the home language preferred to consult in isiZulu. The options for Sotho were largely from those who indicated Southern Sotho, Sepedi or Tswana as their home language. Virtually all who preferred to consult in isiXhosa had indicated isiXhosa as their home language. Notably, the isiXhosa language – which was the dominant ‘home language’ in the sample – was not the preferred language of consultation.
Family income, expenditure on health care and medical aid coverage
There were 2011 responses on monthly family income, which was reported as ‘none’ by 580 (29.0%) of respondents, as
< R1000 by 834 (41.5%) respondents, as R1001 – R3000 by 396 respondents (19.7%), as R3001 – R6000 for 119 respondents (5.9%) and as > R6000 for 81 (4.0%) respondents.There were also significant gender differences in income (Figure 2). Female respondents were more likely to be earning no income or earning < R1000 per month than their male counterparts (75.1% compared to 65.1%). Similarly, more male respondents earned > R3000 per month than their female counterparts. There were 1797 responses with regard to estimated monthly family expenditure on health care: 1122 (62.4%) indicated that they spent < R100, 400 (22.3%) spent R101 – R200, 122 (6.8%) reportedly spent R201 – R300, whereas 153 (8.5%) reported spending > R300 per month on health care. There were no significant gender differences in reported family expenditure on health care. The major means of payment for pharmaceutical services were cash, medical aid and credit facilities. There was an association between the amount spent on health care per month and the mode of payment for pharmacy services; of those who reportedly spent < R 100 per month on health care, 92.6% paid cash. Only 275 (13.9%) respondents had medical aid membership. Those with medical aid cover indicated that their first choice of health provider would be a medical practitioner (GP) (31.3%), pharmacy (26.3%) or a primary health care (PHC) clinic (26.3%), whereas those without medical aid cover stated their choices as a PHC clinic (44.7%), pharmacy (29.4%) and GP (13.9%). The differences in choices were significantly different overall (p < 0.001), with those that had medical aid cover more likely to go to the medical practitioners whilst those without medical aid cover were more likely to visit the PHC clinic. Furthermore, only 9.7% for whom the pharmacy was the first choice in emergencies had medical cover. Overall, however, the choice of pharmacy services was not influenced by medical aid membership.
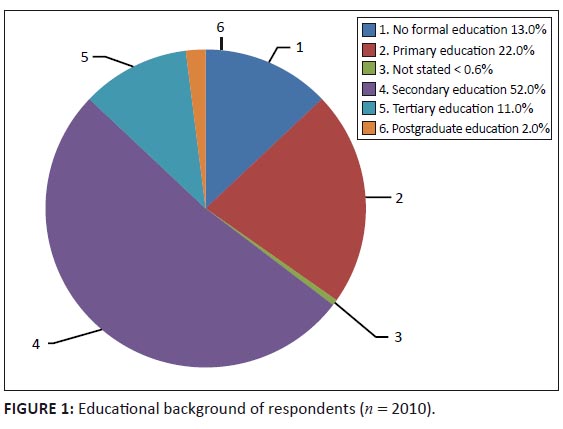 |
FIGURE 1: Educational background of respondents (n = 2010).
|
|
|
TABLE 1: Comparison of home language and language for consultation
preferences amongst the study respondents.
|
Preferred gender of pharmacist
More than a quarter (27.6%) of respondents indicated that they preferred a male pharmacist, 24.9% preferred a female pharmacist, whereas 47.0% had no gender preference. Amongst those with gender preferences, men preferred male service providers, whereas women preferred female service providers. The gender preference for the pharmacist showed no association to the age of the respondents (p = 0.201). However, the education level of the respondents affected the gender preferences, with the uneducated more likely to express a preference. Family income was also associated with gender preference (p < 0.005), with fewer of those in the ‘no income’ or very low income (< R1000 per month) bracket expressing a preference. The respondents’ employment status, however,
showed no apparent association with the gender preferences for the pharmacist.
Convenience of services, including privacy
Most of the respondents (n = 1860, 92.7%) indicated that they would be at ease to discuss any aspects regarding their heath or medication with a pharmacist and this had no apparent association with gender, age, or medical aid membership. However, the level of education, employment status and household income all showed statistically significant association with how at ease the respondents felt when dealing with a pharmacist. Whilst 94.1% of those with no formal education were at ease, only 88.5% of those with tertiary education and 86.1% of those with postgraduate education (p < 0.001) were at ease and only 83.9% of student respondents indicated they would be at ease compared to 91.0% from the other groups (p < 0.001). Fewer of those who spent more on health care (89.6%) were at ease to discuss any aspects regarding their heath or medication with a pharmacist, whereas this varied from 92.1% to 98.0%
(p < 0.001) for the other health care expenditure groups.Regarding the preferred consultation area within the pharmacy, 430 respondents (21.4%) were happy to consult at the front counter of the dispensary, 815 (41.5%) preferred a private consultation area, 222 (11.0%) preferred to consult in the pharmacist’s office, 408 (20.3%) suggested a semi-private area and 115 (5.8%) respondents indicated that it did not matter where the consultation took place. The gender of the respondents had no apparent influence on the preferred area for consultation, but older respondents (> 81 years) preferred private consultation areas or the pharmacist’s office (68.3%) and were less inclined to opt for the front of the counter (7.3%) than the rest. Medical aid membership had an influence on consultation area preferences (Figure 3). Proportionately more of the respondents with medical aid (67.2%) preferred private consultation areas and the pharmacist’s office compared to those without medical aid cover (50.9%). On the contrary, only 10.3% of those with medical aid opted for front of the counter consultation, compared to 23.3% of those without medical aid; these differences were statistically significant (p < 0.001). More than two-thirds (n = 1375, 68.7%) of the respondents preferred pharmacy services between 08:00 and 12:00, 380 (18.9%) between 12:00 and 17:00, 39 (1.9%) between 17:00 and 21:00 hours, whilst for 216 respondents (5.8%) it was various combinations of those periods (e.g. between 08:00 and 17:00). There were differences in convenient opening hours for pharmacies based on medical aid membership, gender, educational level, employment status and means of transport used when seeking health services. For the unemployed, the convenient service hours were stated as 08:00–12:00 by 76.2%, 12:01–17:00 by 16.3%, 17:01–21:00 by 0.9% and later than 21:00 by 6.6%, whereas the respective figures were 64.1%, 25.1%, 4.3% and 6.6% for those in full-time employment, 64.1%, 22.6%, 4.1% and 9.2% for the self-employed, 67.7%, 26.2%, 1.5% and 4.6% for those doing part-time work and 77.8%, 21.4%, 0% and 0.9% amongst students. The employed (all categories) chose the 17:01–21:00 slot more than others and the overall differences were statistically significant (p < 0.001). Whilst 70.5% of those without medical aid cover indicated the most convenient times as the morning slot (08:00–12:00), the corresponding figure for those with medical aid was 57.9% and the respective figures were 18.1% and 24.2% for the afternoon slot (12:01–17:00) – these differences were statistically significant (p < 0.001) (Table 2).
Choice of health care providers
More than one-third (n = 768, 38.2%) of respondents indicated that their first choice of a health care provider was the PHC clinic, 532 (26.5%) the pharmacy, 300 (14.9%) a GP clinic and 37 (1.8%) a traditional healer. A substantial number of respondents (n = 373, 18.6%) provided alternative suggestions, including street vendors (2.0%) and a ‘muti shop’ (1.0%). Gender influenced the choice of health care provider (p < 0.005) – 49.8% of female respondents indicated their first choice of health care provider as a PHC clinic, compared to 41.4% of men, relatively more men (53.1%) chose the pharmacy or GP than women (47.3%) and more men (5.7%) than women (2.8%) opted for alternatives such as traditional healers and/or herbalists or ‘muti shops’.The respondents’ age also influenced their choice of provider (p < 0.001), with those older than 81 years twice as likely as younger age groups to choose the GP (37.8%). In this regard, 17.0% of the 15–30 year age group, 17.7% of the 31–45 year age group, 18.9% of the 46–60 year age group and 17.0% of the 61–80 year age group preferred the GP as first choice. The use of the PHC clinics varied from 51.1% in the 15–30 year age group to 42.1% in the 30–45 year age group, 41.7% in the 46–60 year age group, 39.0% in the 61–80 year age group and 29.7% in the > 81 years age group. Interestingly, the older age groups – 60 years and above – hardly indicated alternatives such as traditional healers, herbalists or muti shops. Employment status affected choice of health care provider to the extent that 66.0% of employed respondents and 64.4% of self-employed respondents indicated the pharmacy and GP as first choice, compared to 42.3% of unemployed respondents. Similarly, 44.1% of the unemployed chose a PHC clinic as first choice, compared to 24.5% of the employed and 22.3% of the self-employed. The monthly expenditure on health care was also associated with these choices (Figure 4). Those who spent > R300 per month were more likely to patronise a pharmacy or GP than those who spent < R100 per month, for whom first choice were PHC clinics. When asked about the health care provider of choice in case of emergency, 743 (37.0%) respondents chose the pharmacy, 25.0% the PHC clinic, 15.0% the traditional healer and 10.0% the GP. There was a statistically significant association between education level and choice of health care provider in case of emergency, with 51.5% of those without formal education choosing the PHC clinic, compared to 52.3% of those with primary school education, 55.4% of those with secondary education, 58.8% of those with tertiary education and 60.9% with postgraduate education (p < 0.001). The pharmacy was the first choice for those with postgraduate education, as well as for those who spent approximately R300 per month on health care, and was the overall favourite in emergencies (37.0%). Clearly, the choice for pharmaceutical services was not affected by medical aid membership in both acute and emergency situations.
Ability and willingness to pay for additional services
The respondents were also questioned about their ability and willingness to pay for health care services, as well as the possibility of using additional services offered by the pharmacies. On the ability to pay for the services, the pattern was the same across the expenditure levels, with 89.3% of those spending < R100 per month, 93.1% of those in the R101 – 200 range, 94.3% of the R201–300 group and 89.0% amongst those reportedly spending > R300 per month on health care stating they would be able to pay (p = 0.062). Similarly, respondents all categories of health care expenditure expressed willingness to pay for additional services, with the respective values of 89.3%, 93.8%, 90.5% and 89.0% responding in the affirmative (p = 0.063). Equally high proportions of the respondents across the health care expenditure groups stated that they would use such services – 93.8% of those spending < R100 per month,
97.5% of those spending R101 – R200, 95.2% of those spending R201 – R300 and 94.8% of those reportedly spending > R300 per month on health care. There was no significant association between gender, age, employment and family income on the one hand and the ability to pay, willingness to pay and possibility of using additional pharmacy services on the other.
 |
FIGURE 2: Percentage comparison of gender versus monthly income of study
respondents.
|
|
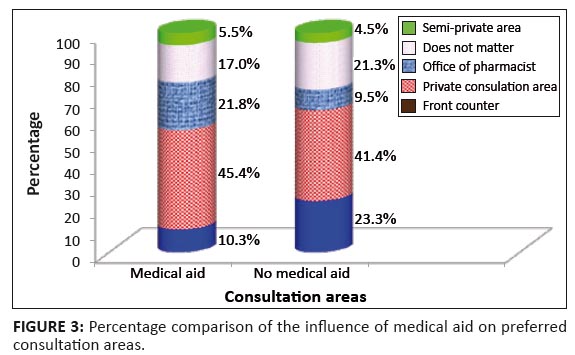 |
FIGURE 3: Percentage comparison of the influence of medical aid on preferred
consultation areas.
|
|
The study protocol was approved by the North-West University (NWU) Faculty of Health Sciences Research Committee. The committee judged the protocol as not requiring separate ethics clearance since it had no direct clinical interventions. The informed consent process was elaborated in the proposal and followed during the study. The purpose of the study was explained to the respondents, after which those who voluntarily agreed to participate signed the informed consent form prior to completion of the questionnaire. No specific respondent could be identified,
thus confidentiality and anonymity of information was maintained throughout the study.
The study was based on established quantitative research methodology and employed a large sample size (> 2000 respondents) to minimise bias and improve the application of the findings to a broader population. Bias was further limited by the fact that the field workers operated autonomously (though under the overall guidance of the researchers); therefore, the latter did not have any influence on the responses given by the community members.
The study tool was validated and piloted prior to being finalised and used in the survey.
|
TABLE 2: Preferred service hours by means of transport and medical aid
membership amongst study respondents.
|
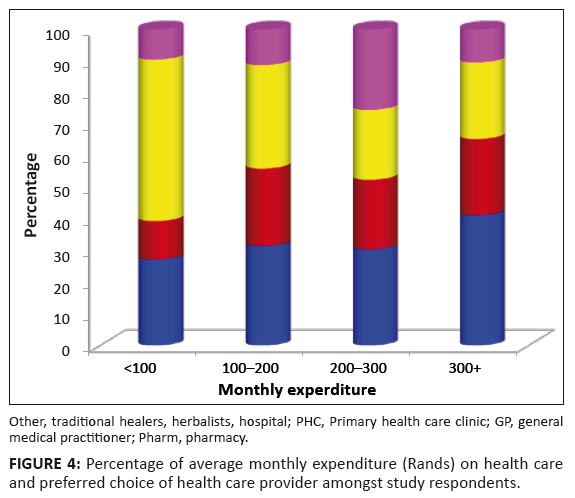 |
FIGURE 4: Percentage of average monthly expenditure (Rands) on health care
and preferred choice of health care provider amongst study respondents.
|
|
There were relatively more female respondents in the survey (54% female versus 46% male) and most of the respondents were unemployed, had secondary school education, spent less than R200 on health care per month, had family incomes of less than R1000 and had no medical aid cover. The choices of health care provider were associated significantly with gender, medical aid coverage, means of transport, level of education, experience of health care, language preference, as well as family income, which is consistent with findings from elsewhere (Kaiser 2000). However, access to pharmaceutical services was not influenced by income levels or medical aid membership and, in cases of emergencies, the pharmacy was the most likely choice for about 37% of respondents. That supports the well-acclaimed easy accessibility of the pharmacists and the pharmacy (South African Pharmacy Council 2007).The finding that medical aid membership affected the choices indicated by the respondents is in line with a significant body of evidence showing that those with medical aid membership in South Africa sought health care services more often than those without medical aid cover (Blecher & Harrison 2006; Dambisya 2005). However, the results indicate that access to pharmaceutical services remain the same regardless of medical aid membership. Significantly, those without medical aid membership or those with low family incomes were more likely to visit PHC clinics, which offer free services to most of the population or charge only a nominal fee (Bamford & Hugo 2001; Bannister 2001, Blecher & Harrison 2006). The preference for PHC facilities in South Africa is also well described, with the medically insured also reverting to the public sector when their medical aid allotment is exhausted (Gilson & McIntyre 2005). Visits to the GP were influenced greatly by income, employment status and medical aid membership, whereas this was not the case for visits to the pharmacy. This finding may be explained by the fact that services from the GP require a consultation fee, whereas consultation services at the pharmacy are free of charge. Furthermore, this finding supports the view that the pharmacist is generally the most accessible of private health professionals (Larson, Rovers & MacKeigan 2002; Lorraine 1999). The finding that those who reportedly spent more than R300 were less likely to use cash for their visits may be
explained by two likely reasons. Firstly, higher income groups are more likely to have medical aid to cover their costs,
whereas lower income groups, who are less likely to have medical aid, will have to pay cash (Still 2007). Secondly, those
who were able to spend more on health care were also found more likely to afford alternative means of payment, such as credit cards,
which are linked to employment status and stable income; moreover, there is an income threshold below which banks do not offer credit
cards (Ricketts 2000b; Still 2007).
That the elderly preferred more privacy should not be surprising, because older persons in the Black cultures of South Africa are traditionally reluctant to discuss their problems in the presence of, or with strangers, especially with those who may be younger than them (March et al. 1999; Sheu 1998). Similarly, the younger respondents and students, tend to have ‘sensitive’ problems, such as those related to sexual and reproductive health, for which they also prefer more privacy. The message for pharmacy owners is to design these facilities in such a way that the need for privacy can be met through private consultation areas (Watermeyer & Penn 2009a, 2009b). The education levels of the respondents per se had no apparent influence on the findings in this study, but it is likely that it had an indirect influence through the employment status, family income levels and medical aid membership, all of which are influenced by the education attainment of an individual (Harvey 2000; Nattrass & Seekings 2001). It was notable that unemployment was higher amongst women, regardless of education, which supports the notion that the employment situation in South Africa remains biased against women (African National Congress 1994). The views on convenient service hours may be interpreted in a number of ways. The majority may have indicated their preference to visit the pharmacy during office hours as a conditioned reaction to established practice; they accept without questioning that this is when the pharmacy is open (Ricketts 2000a; Rogers et al. 1998). It could also be based on the fact that the population for the survey use public transport which tends to be less readily available later in the day and hence the pragmatic preference to visit the pharmacy early in the day. That may also be tied in with the perception of personal safety and higher crime levels in the evenings and night time; hence, most prefer the hours before 17:00. The preferred service hours for the employed may suggest that they have access to more convenient means of transport or live in neighbourhoods close to the pharmacies and could therefore afford to visit the pharmacy late. One of the most remarkable findings is that less than 5% of respondents suggested traditional healers or herbalist as their choice of provider, contrary to the view that the majority of Africans consult traditional healers first – for instance, a recent BBC report stated that ‘an estimated 70% of South Africans will visit a spiritual healer before seeking conventional medical help’ (Hegarty 2011) – whilst Watermeyer and Penn (2009a) say that the majority of Africans undertake dual consultation. Many of the older respondents are likely to have some form of chronic illnesses, many of which are not curable by the medical establishment, an explanation which has been proposed before to make them more likely clients of the traditional healers or muti shops (Larson 2002; Lorraine 1999). Yet the older respondents were found in the present study to be the least likely to indicate such alternative practitioners as their choice of service providers. The present study guaranteed the respondents’ anonymity and confidentiality of any information provided; hence, it is unlikely that the answers to that particular question were biased towards ‘expected’ answers. It is high time we questioned the veracity of some of the statements about how widespread the use of traditional medical practices actually is. The present study was conducted before the Government Employees Medical Scheme (GEMS n.d.,
http://www.gems.gov.za) was implemented. The GEMS made medical aid membership accessible directly to many people across the country, offering lower and more affordable premiums charged by other schemes; consequently, it may be expected that more people in the communities within which this study was undertaken may, in the mean time, have gained access to medical aid membership and hence the patterns favoured by medical aid membership may be more prevalent now than at the time of the study. With the proposed National Health Insurance (NHI), the heath care seeking patterns of the population is likely to change even further, with more people opting for private services such as pharmacies and GPs. It will certainly make these private practices more viable options in poor areas when everyone is covered by the NHI (McIntyre 2010).
The study was confined to five townships of the Gauteng Province, so the findings may not be applicable to other parts of South Africa, such as the Limpopo Province, which has been reported to offer fewer employment opportunities even in urban areas (Provincial Decision-making Enabling Project 2009). The strategy to exclude those who had sought services at health facilities may be seen as a strength of the study, as alluded to above, but because it excluded those who sought health services it limited the responses to only those who were apparently healthy, those who felt they did not need the health services, or those who were unable or unwilling to seek health services at the time they were contacted for the survey. Perhaps the inclusion of those who patronised the different health services at the time of the survey may have provided a different perspective. As discussed above, the study was
conducted before the initiation of the GEMS (which expanded membership to medical aid schemes), so that some of the conclusions arrived at in this study may not be applicable (or at least to the same degree) any longer.
Based on findings from the present study, it is recommended that:• Those in a position to should not hesitate to establish pharmacies in underserviced areas – because the community members are willing and able to pay for the services, pharmaceutical services are viable and sustainable. • Those considering establishing pharmacies in the townships of the West Rand should ensure that they have on staff those that are knowledgeable in the preferred languages of isiZulu and Sotho. • Further research should be conducted to assess the impact of the GEMS on the views of the township communities on access and utilisation of pharmaceutical services in underserviced areas.
Access to pharmaceutical services in underserviced areas, such as those of the West Rand, may be influenced by a variety of factors including family income, medical aid membership, education level, age and gender of pharmacy service provider. However, residents of these areas are willing and able to pay for pharmaceutical services regardless of their income levels. Whilst those without medical insurance were more likely to revert to PHC for their health care needs, the pharmacy was equally accessible regardless of medical aid cover. Taken together,
these findings suggest the need and viability of community pharmaceutical services in such underserviced areas.
The paper is based on work that forms part of the primary author’s PhD research at NWU and the study is supported by the School of Pharmacy at NWU. We are grateful to the fieldworkers who undertook the data collection, to Prof. N.Z. Nyazema and Ms N.E. Furumele for their contributions during the development and finalisation of the research
instruments and to Ms B.C. Coetzee for help with the translation of the Abstract into Afrikaans.
Competing interests
The authors declare that they have no financial
or personal relationships which may have inappropriately influenced them in writing this paper.
Authors’ contributions
D.A.S. (University of Limpopo) participated in all aspects of the study, drafted the paper and finalised it with inputs from the co-authors. J.H.P.S. (North-West University) and M.S.L. (North-West University) supervised the study development and implementation process, guided the data analysis and contributed to the draft and final versions of the paper. Y.M.D. (University of Limpopo) critiqued the data,
helped with the cross-tabulations and made substantial inputs into the draft and the final versions of the paper.
African National Congress, 1994, A basic guide to the reconstruction and development programme, Aloe Communications, Troyeville.
http://dx.doi.org/10.1002/1099-1751(200004/06)15:2<149::AID-HPM584>3.0.CO;2-YBamford, E. & Hugo, G., 2001, ‘Identifying gaps in health service provision: GIS approaches’,
paper presented at the meeting of the 6th National Rural Health Conference, Canberra, 04–07 March. Bannister, C., 2001, ‘Chemist lifts rural retailing’, Retail World 54, 15. Barron, P., 1998, ‘Equity in 1998: An overview’, in A. Ntuli, (ed.), South African health review,
pp. 1–6, Health System Trust, Durban. Blecher, M. & Harrison, S., 2006, ‘Healthcare financing,’ in P. Ijumba & A. Padarath (eds.),
South African health review 2006, Health Systems Trust, Durban, viewed 16 June 2011, from
http://www.healthlink.org.za/uploads/files/chap3_06.pdf Dambisya, Y.M., 2005, ‘Confronting inequities in health service delivery: An overview of
the state of the South African health system’, Journal Of Management & Science 3, 13–23. Department of Health, 1996, National drug policy, Government Printers, Pretoria. Gilson, L. & McIntyre, D., 2005, ‘Removing user fees for primary care in Africa: The need for careful action’, British Medical Journal 331, 762–765.
http://dx.doi.org/10.1136/bmj.331.7519.762,
PMid:16195296
Government Employees Medical Scheme, n.d., Background, viewed 10 February 2012, from
http://www.gems.gov.za/default.aspx?vBR48Vf9KNL7jeeIJMpLEXLCY7A8Hh2rirUmN/aKb7k= Harrison, S., Bhana, R. & Ntuli, A., 2007, ‘The role of the private health sector within the South African health system (editorial)’, in S. Harrison, R. Bhana & A. Ntuli (eds.), South African health review 2007, Health Systems Trust, Durban, viewed 16 June 2011, from
http://www.hst.org.za/uploads/files/editorial_07.pdf Harvey, L., 2000, ‘New realities: The relationship between higher education and employment’, Tertiary Education and Management 6, 3–17.
http://dx.doi.org/10.1080/13583883.2000.9967007 Hegarty, S., 2011, ‘South African woman tells of spiritual healing temptation,’ BBC World Service, 26 April, viewed 20 June 2011, from
http://www.bbc.co.uk/news/world-africa-12883247 Kaiser, C., 2000, Optimising the location of services: The case of pharmacies in Western Australia. Unpublished MPharm thesis,
School of Medical Sciences, University of Adelaide. Larson, L.N., Rovers, J.P. & MacKeigan, L.D., 2002, ‘Patient satisfaction with pharmaceutical care: Update of a validated instrument’, Journal of the American Pharmaceutical Association 42, 44–50.
http://dx.doi.org/10.1331/108658002763538062,
PMid:11833515
Lorraine, P. 1999, ‘The development of a sustainable health service in a small rural community: Every
cloud has a silver lining’, in H. Pampling & G. Gregory (eds.), Leaping the Boundary Fence:
Using Evidence and collaboration to build healthier rural communities,
5th National Rural Health Conference proceedings, Canberra, Australia, 14–17 March 1999, pp. 504–509. March, G., Gilbert, A., Roughead, E. & Quintrell, N., 1999, ‘Developing and evaluating a model for pharmaceutical care in Australian community pharmacies’, The International Journal of Pharmacy Practice 7, 220–229.
http://dx.doi.org/10.1111/j.2042-7174.1999.tb00973.x McIntyre, D., 2010, ‘National Health Insurance: Providing a vocabulary for public engagement’, in S. Fonn & A. Padarath (eds.), South African health review 2010, pp 145–156, Health Systems Trust, Durban: viewed 15 June 2011, from
http://www.hst.org.za/publications/876 Nattrass, N. & Seekings, J., 2001, ‘“Two Nations”? Race and economic inequality in South Africa today’, Daedulus 130, 45–70. Parliament of South Africa, 1950, The Group Areas Act (Act No. 41 of 1950), viewed 15 May 2012, from
http://africanhistory.about.com/library/bl/blsalaws.htm Provincial Decision-making Enabling Project, 2009, A profile of the Limpopo Province: Demographics, poverty, income, inequality and unemployment from 2000 till 2007, Background Paper 1(9), PROVIDE Project, Johannesburg Ricketts, T.C., 2000a, ‘The changing nature of rural health care’, Annual Reviews of Public Health 21, 639–657.
http://dx.doi.org/10.1146/annurev.publhealth.21.1.639,
PMid:10884968
Ricketts, T.C., 2000b, ‘Health care in rural communities: The imbalance of health care resource distribution needs correction’, Western Journal of Medicine 173, 294–295.
http://dx.doi.org/10.1136/ewjm.173.5.294,
PMid:11069850
Rogers, A., Hassell, K., Noyce, P. & Harris, J., 1998, ‘Advice-giving in community pharmacy: Variations between pharmacies in different locations’, Health and Place 4, 365–373.
http://dx.doi.org/10.1016/S1353-8292(98)00031-8 SAS® version 9.1, 2008, computer software, SAS Institute Inc., Cary. Sheu, B.J.K., 1998, ‘Giving patients privacy in the pharmacy’, American Journal of Health
System Pharmacy 55, 2244–2246. South African Pharmacy Council, 2007, ‘Services for which a pharmacist may levy a fee’,
Pharmaciae 7 (April–July), 14. Still, L., 2007, ‘Out of pocket health care costs rub salt in the wound,’ Sunday Times, 12 August, viewed 10 June 2011, from
http://www.suntimes.co.za Tshabalala-Msimang, M., 2001, ‘Message to the PSSA Conference from the Minister of Health, Dr Manto
Tshabalala-Msimang’, South African Pharmaceutical Journal 68, 9–10. Van Rensburg, H.C.J. & Pelser, A.J., 2004, ‘The transformation of the South African health system,’
in H.C.J van Rensburg (ed.), Health and healthcare in South Africa, Van Schaik Publishers, Pretoria. Watermeyer, J. & Penn, C., 2009a, Working across language and culture barriers: Communications skills for Pharmacists,
Paediatric Aids Treatment for Africa, Cape Town. Watermeyer, J. & Penn C., 2009b, ‘Communicating dosage instructions across cultural and linguistic barriers:
Pharmacist-patient interactions in a South African antiretroviral clinic’, Stellenbosch Papers in
Linguistics PLUS 39:107–125. World Health Organization, 1988, The role of the pharmacist in the health care system. Report of a WHO
Consultative Group, New Delhi, India, 13–16 December 1988, Document No. WHO/PHARM/94.569, World Health Organization, Geneva.
|
